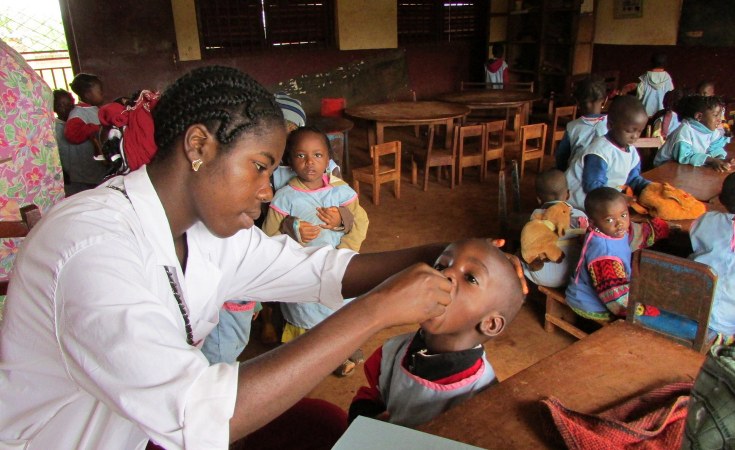
As we mark Africa Vaccination Week and World Immunization Week, the World Health Organization, the Gates Foundation, the Global Alliance for Vaccine and Immunization (GAVI) and partners can point to significant progress. Thanks to vaccination efforts, there was for example an 84% drop in measles deaths between 2000 and 2016 worldwide.
Global vaccination coverage has however stalled at 86%, with little progress over recent years. In 2016, an estimated 19.5 million infants worldwide were not reached with routine immunization services such as DTP3 vaccine. Around 60% of these children live in 10 countries: Angola, Brazil, the Democratic Republic of the Congo, Ethiopia, India, Indonesia, Iraq, Pakistan, South Africa, and my native Nigeria.
In Nigeria, I have worked with midwives and partners to educate families about the importance of vaccination and raise alarm at the lack of coverage. GAVI has revealed that despite considerable investment - of about $700 million – in Nigeria we only have immunization coverage of around 30%.
Our Well Being Africa Foundation midwives work closely with women in their antenatal and postnatal classes as educators, but they have experienced how mothers and infants are being let down by a lack of coverage. We must prioritise maternal vaccines – tetanus, the anti-D injection for all pregnant women with rhesus negative blood, and HPV catch-up for adult women to protect against cervical cancer. Nigeria is not yet vaccinating for HPV as a matter of routine, and yet cervical cancer along with breast cancer are the biggest killers of women in my country after death in childbirth. The public health sector has only two radiology machines in the entire country that are operational, both at National Hospital in Abuja. One is current working. whilst the other will be commissioned soon. That is not sufficient to serve a country of 198 million people. With only one radiology treatment machine currently functioning, it is in Nigeria's best interest to urgently invest in prevention through vaccination.
Low vaccination rates are a national health emergency and a global health security issue
Prevention is better than cure – but currently most of our citizens are receiving neither.
The rate of immunization should be treated as a national health emergency and a global health security issue. It is time that we took the lead domestically. As Dr Tedros Adhanom Ghebreyesus, the first African Director-General of the WHO stated last week in his keynote IMF/WBG Spring Meetings speech, we must focus on mobilising domestic resources and consider external input as supplementary. Frontline healthworkers, like our MamaCare midwives, are best placed to lead this battle and will do so with political will and support from Government.
Vaccinations have the ability to protect not just an individual, but a community. An increase of vaccine coverage in low- and middle-income countries by 2030 would prevent 24 million people from falling into poverty due to health expenses. Health workers' efforts to increase immunization builds, therefore, the foundation for strong primary health care and is a route to universal health coverage. The desire for health for all, based on blanket vaccination coverage, is overwhelming – but families are currently being let down.
Toyin Saraki is Vaccine Champion for Women Advocates for Vaccine Access and Founder-President of the Wellbeing Foundation Africa. She is Global Ambassador for @world_midwives ,