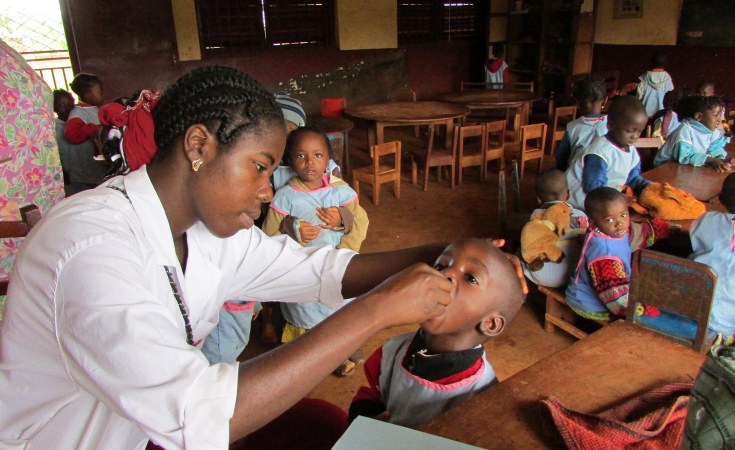
In February, PREMIUM TIMES exclusively spoke with Chris Elias, the President of the Global Development Division of the Bill and Melinda Gates Foundation and Paulin Basinga, the foundation's country director, on the role the foundation played in the eradication of wild polio in Nigeria and a range of other developmental issues.
What role did the Bill and Melinda Gates Foundation play in the eradication of polio in Nigeria and what is your assessment of the campaign against polio?
Chris Elias: Finishing the job on polio eradication globally is one of the priorities of Bill and Melinda Foundation - has been really from out start. The Bill and Melinda Foundation has been around for about 20 years. The global effort to eradicate polio started in 1988 when the world health assembly - all governments of the world - committed to eradicating polio. They made very fast progress in many places. By 2000, only five countries were left with polio. The last 20 years have been challenging because the last mile, as we call it, is the most difficult.
The last cases here in Africa have been in Nigeria. In the last five and a half years, there have only been four cases in Africa, in Borno in 2016. We went two years without any cases then we had these four cases pop up in 2016. How did we know we were vulnerable? At that time, we were missing, because of the conflict in the North-east, probably half a million kids. Over the last three years, it's been 40 months since the last cases of wild polio in Nigeria or anywhere else in Africa. Extraordinary efforts are being made by the government of Nigeria, particularly the governors of the northern states to reach the unreached children so as to ensure that everybody is immunised against polio.
Follow us on WhatsApp | LinkedIn for the latest headlines
To give you a sense of the progress, in 2016 we are missing probably a million kids. Today, our estimate is about 34,000 kids that have not been immunised in Borno. The efforts of Governor Shettima (immediate past governor of the state) and now Governor Zulum have been extraordinary in putting a partnership together with UNICEF, Bill and Melinda Gates Foundation and Dangote Foundations and importantly, the vaccinators. The army protects the vaccinators to have access to most of the children and as a consequence, we haven't seen any wild poliovirus in 40 months. We've increased our environmental surveillance, increasing the confidence that we have, in fact, and interrupted wild polio in the North-east, in Nigeria and in the continent.
The way it works is that World Health Organisation has an African Regional Certification Commission, an independent body; they will make recommendations to the World Health Organisation about whether the fact they are confident that Africa is free of polio and we expect them to make the recommendation by June of this year. The longer we go without the risk of polio and the stronger our surveillances, the more confident we are. So, we are anticipating a favourable recommendation from the certification commission as early as June of 2020.
Can you tell Nigerians some of the most effective strategies your organisations used and what sort of help was provided by the federal and state governments?
Chris Elias: The Gates Foundation is a significant funder of the Global Initiative for Polio Eradication. We provide about a third of the funding for that global initiative here in Nigeria and other places like Afghanistan, Pakistan and many other vulnerable countries. We provide funding, but also provide technical assistance. One of the thing about the 30 plus years journey of polio eradication is we have learned how to do it in other places. We brought some of the innovations that helped us succeed in India which is one of the countries that recently eradicated polio. We brought some of the innovations here, particularly, using the Emergency Operation Centres. We've supported Emergency Operation Centres at the federal level in Abuja and at the state level in northern states. The Emergency Operation Centre here is a place where all the partners have come together as one team - the government, the World Health Organisation, UNICEF, everybody working on this - with real-time information and data on surveillance, on the quality of the campaign, outreach, etc. That teamwork combined with the use of data to continually improve the quality of the outreach and the campaign, knowing which children you are missing and innovative ways of reaching them have been critical to the success. It worked in India, it's now working in Nigeria and we are using same approaches that have succeeded here in Nigeria to work in the final frontiers of polio eradication, which is in Pakistan and Afghanistan.
Everywhere we work, we have to work with the local traditional and religious leaders and community leaders in general. That has been particularly important here in Nigeria, in the north, where 15 years ago we heard rumours about the vaccines that were incorrect, causing people to hesitate about the vaccines. We and the World Health Organisation committee members in Northern Nigeria are not as effective as having their local imams, their local traditional leaders - people they trust, people who they go to every day for advice - to tell them it is a safe vaccine that protects them from paralysis and death. You can trust the government in a partnership to give those vaccines to children. The participation of the Sultan of Sokoto, the Emir of Kano, the Emir of Zauzau have been critical in helping us reach the final mile and get every child vaccinated.
After taking polio down, what other big challenge in the country are you planning to take on?
Chris Elias: About winning the polio battle, the battle is not won until it's gone everywhere. Even if we succeed as I think we will in certifying Africa polio-free, as long as there is wild poliovirus circulating in Pakistan and Afghanistan, Africa remains vulnerable. To protect against that, we have to keep at it until we are done globally to make sure children are immunised. One of the reasons it's been so hard to fight the last battle against polio in Africa is the overall immunisation rates for children are persistently low, particularly in the north. In Sokoto for instance, less than 10 per cent of the children received the first suite of vaccines. Vaccines are lifesaving against, not just polio but pneumonia, diarrhoea and other infectious diseases. The natural progression from finishing the job of polio eradication is to strengthen the routine immunisation system, make sure that Nigerian children are benefiting from the first suite of thirteen different vaccines that protect them against a wide array of illnesses and to ensure that should someone travel from here to polio-endemic areas like Pakistan, that the children won't get infected and have polio reintroduced into Africa.
The certification of Africa as wild poliovirus free will be an important milestone, one hard-fought for four decades. Africa will remain vulnerable as long as there is polio circulating in Afghanistan and Pakistan. The way that continues to protect African children is to make sure that they get all of the vaccines. A natural extension of our work on polio eradication is that we are working with the governors in the north, as well as the national governors' forum, to talk about the importance of routine immunisation, to talk about how to protect women and children against all of the vaccine-preventable illnesses.
The natural extension of that is we need to focus on the primary healthcare system. The primary healthcare system is the first line of the healthcare system where people can go to get 80-90 per cent of their healthcare needs met. A well-functioning primary healthcare system delivers vaccines, provides women with contraceptive choices, it treats children who are sick quickly so that they don't need more advance care, it provides nutritional supplements to keep children healthy. Strengthening the primary healthcare system has become the main focus of our health work in Nigeria. It's a natural progression for winning the fight on polio, to expanding to broad immunisation to looking at how we can comprehensively address the health needs of women and children in all the communities in Nigeria.
What do you think NGOs, government and Nigerians generally should do to roll back the frightening statistics of infant and maternal mortality in Nigeria?
As you said, the primary healthcare system in Nigeria is pretty weak. It is characterised by a couple of things. One is under-investment by the government, which leaves people dependent and getting cured primarily by paying from their pockets, which is very difficult for poor people to do. As a consequence, the system lacks sufficient trained health workers. What I am encouraged by, however, is WHO has recognised that in trying to address the healthcare needs of Nigeria, we need to focus more on primary healthcare system.
This is not a unique problem in Nigeria. Most poor countries now spend too much money on tertiary care and not enough on the primary care system. On average, poor countries spend only about a third of their budget on the primary healthcare system even though the primary health care system can address 80-90 per cent of the problem.
Making more informed decisions about how to allocate, I guess the simple way to put it is that governments, including Nigeria, should spend more on health, and the more they have should be spent on where it is most effective, which is the primary healthcare system. One of the things we've been doing together with the Aliko Dangote Foundation is working in a number of states to understand their primary healthcare system, their weaknesses and how to strengthen it.
You mentioned your perception of the primary health care facilities. Facilities are important parts of the primary health care system, but a building is a building. In addition to having facilities and having them in the right places, you also need healthcare workers in sufficient numbers and with sufficient training. You need the medicines, the vaccines and you need the supply chain of medical commodities that don't stick out. If I walk 10 kilometres to a medical facility that doesn't have medicine, I am not likely to walk there again especially if it is hot.
In addition to that, you need funds. The system has to have enough money. I have visited some primary healthcare centres where they have no budget. without the budget, they can't get the medicine, they can't pay the workers, etc.
You also need information, you need to know who you are reaching and who you are not reaching. Finally, you need patients to show up. If you have a system, this is a problem they face particularly common in rural areas, the system is not functional for some time. People don't go there because they have no expectations. If they go there, there is no one there, they have no medicines, there is no money. What they do is, go to the traditional healers, they use money out of pocket to pay for things that may or may not work. So there is a chicken and egg problem where the system has to become functional enough to earn the credibility of the community. So, the community knows I can go there, there will be a nurse, there will be medicine if my child is ill. You have to get all of those things right. You have to have the facilities, the money, the medicine, the workers and the patients. And then you need to use the information to know this patient is coming, we have this problem, we have to adjust our training, we have to adjust our supplies. It is a challenge because it's a very complex system. So, a lot of the partnerships we have with the governors' forum, with specific governors of specific states and the Aliko Dangote Foundation, is understanding that complex system, and how to improve all those dimensions so ultimately we are providing effective primary healthcare to the large population of Nigeria.
Let's talk about something at the core of what the Gate Foundation does - family planning. In 2050, the population of Nigeria is projected to grow larger than the population of the United States to become one of the top three most populated countries in the world. We are growing faster than our GDP, what is your foundation doing in this area?
Chris Elias: People everywhere believe that children are a gift and all the religion I know think we have an obligation to keep children healthy. The discussion around family planning and birth spacing is how to make sure women and children are healthy. Women can have as many children as they want but if they have them too soon, one after the other, it's bad for their health, they become anaemic, they could die in childbirth and it's bad for their children's health - they become stunted and don't achieve their potentials, physically or cognitively. I've had discussions in the north with traditional and religious leaders and say they want women to make their choices. Mostly, we want children to remain healthy and to be healthy, I and the traditional leaders in the north said that if children are not to be malnourished, they have to increase the time between each birth.
You can still have eight children but space them. If you have them too soon they won't be that healthy. So, providing women the opportunity to decide how many children to have, when to have them and means to space them so that she and the children are healthy is consistent with the beliefs of most religions.
The second thing is that there have been a lot of interests in population growth. If you look carefully today, there are three things that increase population growth; the first is families that want to have many children - more than five. They are relatively few and they live in places where child mortality is now very high. Most of these children are dying before their fifth birthday. We know from development experience around the world that we can't bring down the fertility rate without bringing down first, child mortality rate. In those places with very high child mortality, the first step is to improve the children's health; improve the confidence that parents have that their children are going to survive. So, the basic immunisation, nutritional requirements are quite critical. If child mortality stays high, fertility will stay high. That is pretty clear. That is actually, however, the smallest driver of population growth.
The second driver, and is easily addressed is to provide women who want to space children with the means to do so. Right now, we estimate that there are over 210,000,000 women who want to either space their birth or limit their birth but don't have the means to do so. That is easily addressed by making available contraceptive services. Contraceptive methods are relatively inexpensive, they can be readily provided by a functional primary healthcare system, The quickest thing to do is to meet the already expressed interests in limiting births for women who already want to space their children.
The third and most interesting pieces that usually get missed, has to do with the age structure of the population. The fact that half of Nigerians are under the age of 25. And they have long reproductive lives ahead of them. Given the shape of that population, even if each family has 2 children, the population will continue to grow because we're such a young population. So what do we do? There are two things that are quite critical. One is to work on youth employment, to give people meaningful livelihoods.
The second, and this is the most critical, is that the only way you can slow population growth is to space generations as opposed to spacing births. How do you space generations? You educate them. If you provide strong education for women and girl and ensure gender quality, what happens naturally is women start having families later in life instead of having first births at15 as against first births at 25. That shift in the age of the first births essentially spaces the generation and slows population momentum. The biggest driver of population growth is actually the age structure of the Nigerian population and the best way to slow that is to invest in women empowerment, growth and education.
Let's take a trip to Borno State. Nearly a million children there are malnourished. The conflict there has helped to fuel malnourishment. What is the Bill and Melinda Gates Foundation doing to address malnourishment in the region?
Chris Elias: The biggest challenge in Borno is the conflict. They are extraordinary circumstances, the insecurity that disrupts the primary healthcare system, disrupt agriculture productivity. It is very hard to achieve the easily achievable gains of primary healthcare in places that are suffering from conflict and displacement. We see that in Syria today, we see it in Yemen, and we see it in north-eastern Nigeria. In spite of that, some gains are being made.
A big part of our partnership with the Aliko Dangote Foundation is focused on nutrition. We work with them on polio and primary healthcare but we also work specifically on nutrition and to improve the quality of food, their fortification with micronutrients, etc. Delivering ready to use therapeutic foods to treat several cases in the effort to improve the severe case of acute malnutrition and improving the micronutrient content of the food is important.
Part of the efforts of the Bill and Melinda Gates Foundation in Nigeria has been working on improving agricultural productivity. We have, through the International Institute of Tropical Agriculture in Ibadan, quite a broad range of activities in Nigeria on improving yields and productivity of smallholder farmers, which are a very large proportion of Nigeria's population.
We've seen successes of that, even in the north-east and in places that we don't have as much conflict like Adamawa and Taraba, you see significant gains in productivity from a better seed system and agricultural inputs. Those things can help in Borno as well. The Gates Foundation is investing in the agricultural sector in Nigeria as well as to provide more relief to curb malnutrition through our partnership with the Aliko Dangote Foundation.
Affter the huge amount is spent of developmental programmes and people like you dedicate time away from family and loved ones working to achieve these goals, don't you get frustrated sometimes that these problems have seemingly refused to go away?
Chris Elias: Well, if you got a magic wand, I will take it (laughs). One of the challenges I think we have is that the people don't appreciate how much success stories we've recorded. If you step back and look at the progress in the last one year, we've seen child mortality worldwide coming down. In 2000, over 10 million kids died before their fifth birthday. Today, just about 5 million. The progress in reducing child mortality is not as much as we like because there are still kids who die, who shouldn't. We've made tremendous progress, look at the case with the HIV/AIDS, 15 to 20 years ago, HIV/AIDS was a death sentence. Most people had no antiretroviral therapy, most people now live a long reproductive life. Malaria deaths have been cut in half in the last year. Yes, there are days where I feel frustrated but if you step back and look at the success of the lives saved, and the productivity gain, and the economic impact in the communities and countries in Africa, you'll get up and do it again.
Paulin Basinga: l'll like to speak specifically about Nigeria. If you look at the past few years despite all the problems, I think we are seeing some progress. The trajectory is becoming more and more positive. Just to give you a number. five years ago, only 30 per cent of Nigerian kids were vaccinated. Now, the number went up to 51per cent. We need to get to 80 per cent and plus. But that positive trend is amazing. As a development actor, when you go to the villages, you meet the people, you see the resilience in people, you see how much people are demanding change. Their voices are coming out more and more. They know what they need. I think there's a chance that one day, state after state, LGAs after LGAs, you can see some change.
There are some amazing leaders we work with that personally inspire me. When you see the work that Dr Chikwe is doing at NCDC, Nigeria is more prepared now than when Ebola came. Chris talked about how we supported the EOCs (Emergency Operation Centres) in six states, the small amount of money we put into NCDC, Dr Chikwe has been able to put EOC in almost all of the states. They are operating now. When you see the work that Dr Faizal is doing at NPHCDA, you see the change that is happening within that organisation. That gives us hope that there are possibilities to really change this country and when Nigeria will change, it will change all Africa.
No one could imagine that we'd be here for more than three years without a case of one polio bias, even though we still have some derived polioviruses going out there. When you look at the quality of surveillance that the government and partners have put here, to really detect and the fact that we are not detecting any wild polio shows that the severance that we have put in place is strong and many people are learning here. Let me just close by saying millions of health workers are working in very hard situations, in Borno, Yobe. Every day, they wake in the morning, go to the facilities and try to do their bests. That gives us hope.