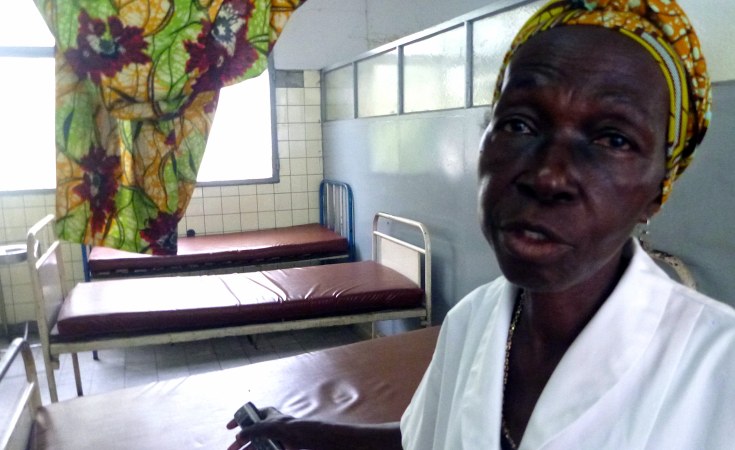
Kinshasa — Her limbs flaccid, her eyes wide with fear and pain, Théthé's cries seem oddly detached from her body, as if part of her isn't lying on a brown vinyl mattress, slick with blood and amniotic fluid, in one of the worst places in the world to be a mother.
The final hours of Théthé's pregnancy have been difficult. Her placenta has torn away from her uterus and her child is being starved of oxygen. In the meantime, Théthé has developed a fever.
She moans and lets out a sharp cry. "Softly, softly," a nurse coaches her.
Théthé groans and pushes, giving birth to a little girl. It is her sixth child. The nurse holds up the waxy baby by the feet. Her arms hang limp, her skin an opaque bluish-pink.
Follow us on WhatsApp | LinkedIn for the latest headlines
"Stillborn," says Kavita Masenga, the lead obstetric nurse. Théthé's moans turn to whimpers. She motions with her hand that she doesn't want to see the baby.
This is not an extraordinary day at Kinshasa General Hospital, the main referral hospital in the capital of the Democratic Republic of Congo (DRC). The most serious obstetric cases from across this traffic-clogged city of 10 million people are sent here. Although conditions have improved in recent years, the hospital remains plagued by the country's problems: power cuts, outdated equipment, poorly paid staff and a lack of drugs.
Years of corrupt leadership, conflict, military-led looting sprees and general deterioration have taken a toll. National elections last year, which were widely criticized as fraudulent, have cast doubts on the government's commitment to change the corrupt ways of the past and focus on the well-being of its citizens.
It wasn't always so bleak at this sprawling medical facility, at least for those fortunate enough to have access to it. Kinshasa General - then named Mama Yemo after the mother of late president Mobutu Sese Seko - once hosted the largest maternity ward in all of sub-Saharan Africa, with up to 150 births a day. Supported by American doctors, patients came from all over the continent to seek care at the hospital, but not any more.
"We used to prepare better with prenatal consultation, and we followed through until the woman gave birth," says Masenga, who has worked at the hospital for more than 30 years. "But now there are very few women who leave the house and come here directly. Often they go to a small health center, and if there is a complication they come here. Sometimes they arrive too late."
Wealthy Nation, Dying Mothers
The DRC is one of the most dangerous countries in which to conceive. Over her lifetime, a Congolese woman faces a one in 24 chance of dying from complications of pregnancy or childbirth. The country is one of six that account for half of all deaths from maternal causes globally. In its annual "State of the World's Mothers" report released on Tuesday, the charity Save the Children listed the DRC among the 10 worst places in the world to be a mother. Eight of the countries are in sub-Saharan Africa.
Some progress is being made, but the decrease in maternal deaths is only about 1.7 percent a year in Congo, compared to an annual 5.5 percent mortality reduction needed to meet United Nations goals for the country by 2015. The death rate is highest in the mineral-rich eastern part of the country, where conflict has flared again this month and rape is a common weapon of competing militias.
In several interviews with medical workers in Kinshasa, they all cited poverty as the main trigger of maternal deaths. Three quarters of Congolese women who did not give birth in a health facility cited lack of funds to pay for services as the reason, according to a World Bank survey.
"In some places, when you arrive [for care] and you don't have money, they just transfer you and transfer you. That is part of the reason we have such a high rate of maternal mortality in our country," says Dr. Blandine Aveledi, reproductive health manager for the New York-based International Rescue Committee (IRC) in Kinshasa. "The greatest problem is access to finances."
Outside the capital, lack of infrastructure poses additional burdens for pregnant women. In rural areas of the country, which is as large as Western Europe, both clinics and the means to access them - namely roads - are negligible. Nearly 80 percent in the World Bank survey said that either distance from a clinic or lack of transport to get there impeded their access to care.
Trained medical staff are also scarce - about one doctor for every 9,000 people. Yet a clean facility and sterile supplies, or even a skilled birth attendant, could cut the rate of both mother and child deaths significantly.
Hard-pressed Congolese health professionals say the country should do better. It possesses vast quantities of diamonds, gold, copper, timber, rubber and other resources. But it ranks at the bottom of United Nations indicators for human development. According to the World Bank, Congo is one of only nine countries where life expectancy has fallen below 1970 levels.
"You cannot tell me my government is so poor, when I see [government] ministers and the number of cars they have, the numbers of villas. When I see that - you want to tell me that they don't have money for the health problems in the country?" says an indignant Dr. Mbwebwe Kabamba, head of the emergency department at Kinshasa General.
Saving Lives Means Spacing Births
Health experts say that closely-spaced pregnancies are one of largest factors in both maternal and child deaths, regardless of whether a woman has access to health care. But only six percent of women use modern methods of contraception, according to Save the Children.
The secretary general in the Ministry of Public Health, Dr. Pierre Lokadi Otete Opetha, says about five percent of the country's budget last year was set aside for health care. This compares with between 15 and 20 percent for developed countries and is well below the minimum figure agreed by the 2001 Abuja Declaration which committed African government to allocate 15 percent of their national budgets to health.
But Opetha insists his government is committed to improving maternal health in the DRC. He says expanding family planning services, which would save lives of both mothers and babies, is a major focus.
"It's a priority of the head of state [President Joseph Kabila]," he says. "I remember at many meetings that he comes back to that. As there is the high-level political will, and with our partners, I think from this year there will be a kicking off of family planning efforts."
The average Congolese woman bears six children. For women who survive pregnancy and childbirth, each new baby increases her family's struggle to feed and educate its children. The more closely one child follows another, the higher the rate of malnutrition, the higher the incidence of malaria and other deadly diseases, and the more difficult for the mother to breastfeed - a proven method of reducing infant deaths.
Medical workers at Kinshasa General say they give advice on family planning to every woman who comes through the maternity ward, but few take it. The reasons are many.
"There is the influence of religion," says Dr. David Bamba, head of the hospital's obstetrics department. "Many sects don't accept one method or another of contraception because they see it as a transgression against divine law."
Apart from religion, there are also myths related to birth control. Many people believe contraception means they will never be able to have children. Some men think it will make a woman promiscuous. And many women believe if they do not produce children their husbands might find wives who are more fertile.
One program, sponsored by the IRC, trains medical workers in maternal health care and how to give advice on contraception.
"At the beginning there was a certain resistance because of lack of information," says Dr. Christian Bitwayiki Semapfa, a doctor from the eastern province of North Kivu, who works for the program. "But everyone came to understand it was a problem that includes everyone, and the husband needed to be involved in family planning. It concerns the wellbeing of not only the woman, but the husband, the family and the whole community."
He said one man in the community had 15 children and was so convinced of the need for birth control that he underwent a vasectomy.
At the Roi Baudouin Hospital in a crowded suburb of Kinshasa, 33-year-old Olivie Kasongo just had her second set of twins. Now she has seven children, and the family lives on a policeman's salary of about U.S.$30 a month.
"It is very difficult because the children - you must educate them, feed them," she says. "I'll come back to [the hospital] to do the family planning. I'm going to speak to my husband and he must accept it."
But the reality is, doctors say, he most likely won't.
Abortion is illegal in the DRC, leaving women who seek it vulnerable to back-alley procedures that routinely cause hemorrhage, infection and death. For most women, however, it is their only alternative to repeated, closely spaced - and hazardous - pregnancies.
Until family planning becomes more widely available and more widely used, abortion will likely remain the leading method of birth control, health workers say. And until then, they say, Kinshasa General will continue to see a steady stream of mothers like Théthé. She narrowly survived the birth of her stillborn daughter, but with each new pregnancy comes more risk.